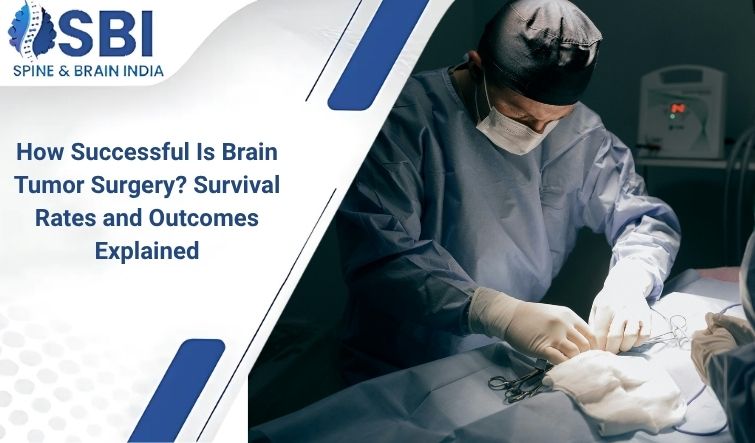
Receiving a brain tumor diagnosis is a life-altering moment that brings a wave of uncertainty. Naturally, the most pressing question for patients and their families is: How successful is brain tumor surgery? Survival rates and outcomes explained in simple terms can help provide the clarity needed to make informed healthcare decisions. Success in neurosurgery is no longer just about survival; it is about preserving the quality of life, restoring function, and preventing recurrence. With modern technological advancements, the success rates for brain tumor removals have improved significantly, offering new hope to patients worldwide. At العمود الفقري والدماغ الهند , we combine surgical expertise with cutting-edge technology to ensure the best possible outcomes for our patients.
What is Brain Tumor Surgery Success?
In the medical world, “success” is a multifaceted term. When discussing how successful is brain tumor surgery, doctors look at several key indicators. First is the “total gross resection,” which means removing 100% of the visible tumor. Second is the preservation of neurological function—ensuring the patient can still walk, talk, and think clearly after the procedure. Lastly, success is measured by the length of time a patient remains “progression-free,” meaning the tumor does not grow back. Because every brain is unique, success is often a personalized metric tailored to the specific type and location of the tumor.
Reasons for Undergoing Brain Surgery
Surgery is frequently the primary treatment for brain tumors because it offers immediate results that other therapies cannot match. The main reasons include:
- Mass Effect Reduction: Large tumors press against brain tissue, causing severe symptoms. Removing the mass relieves this pressure instantly.
- Accurate Grading: A surgical biopsy is the only way to know the exact genetic makeup of a tumor, which dictates the rest of the treatment plan.
- Seizure Control: Tumors often irritate the brain’s electrical pathways. Surgery can significantly reduce or eliminate seizure activity.
- Cure Potential: For many benign tumors, surgery is the only treatment required to achieve a complete cure.
Common Symptoms Leading to Surgery
Patients often find their way to a neurosurgeon after experiencing persistent neurological issues. Recognizing these early is key to a successful outcome:
- Chronic, severe headaches that are worse in the morning.
- Sudden changes in vision or hearing.
- Loss of balance and frequent falls.
- Cognitive changes, such as memory loss or confusion.
- Weakness in a specific arm or leg.
- New-onset seizures in adults.
The Role of Diagnosis in Predicting Success
A successful surgery begins long before the first incision. Advanced diagnostic tools allow surgeons to create a virtual roadmap of the brain.
- High-Tesla MRI: Provides high-resolution images to differentiate between tumor cells and healthy brain tissue.
- DTI (Diffusion Tensor Imaging): This maps the “white matter” tracts, which are the brain’s wiring, ensuring the surgeon does not disconnect vital communication pathways.
- Pet Scans: Help determine the metabolic activity of the tumor, indicating how aggressive it might be.
Modern Treatment Options and Success Factors
The method used to remove a tumor greatly impacts the question of how successful is brain tumor surgery. We now have various tools that make surgery safer and more effective:
- Neuronavigation: Think of this as GPS for the brain. It allows the surgeon to see exactly where their instruments are in relation to the tumor in real-time.
- Intraoperative MRI (iMRI): This allows the surgeon to take an MRI خلال the surgery to see if any microscopic tumor bits remain before closing.
- Fluorescence-Guided Surgery: Patients drink a special dye (5-ALA) that makes tumor cells glow under a specific light, helping the surgeon remove hidden cancerous cells.
- Endoscopic Surgery: For tumors near the base of the skull, surgeons can use small tubes through the nose, avoiding large incisions in the scalp.
Survival Rates and Outcomes Comparison
Survival rates vary significantly based on the tumor’s “grade” (how fast it grows) and the patient’s age. Benign tumors have a near-perfect survival rate, while malignant tumors require more complex, multi-stage care.
Outcome Expectations by Tumor Type
| نوع الورم | Typical Success Goal | 5-Year Survival Rate (Approx.) |
|---|---|---|
| Meningioma (Benign) | Complete Removal | 90% – 95% |
| ورم العصب السمعي | Nerve Preservation | 95% – 98% |
| Low-Grade Glioma | Max Resection / Control | 70% – 85% |
| الورم الأرومي الدبقي (GBM) | Life Extension / Quality | Varies by Genetics |
| ورم الغدة النخامية | Hormonal Balance | 95% + |
Risks and Side Effects of Surgery
While we focus on success, it is vital to understand the hurdles. Every brain surgery carries inherent risks that must be weighed against the benefits:
- Brain Edema: Swelling is common after surgery and is usually managed with steroids.
- Neurological Deficits: Depending on the tumor location, there may be temporary weakness or speech changes.
- Infection or Bleeding: Standard surgical risks that are minimized in sterile, high-tech environments.
- CSF Leak: A leak of the fluid surrounding the brain, which may require additional care to seal.
Recovery and Enhancing Your Outcome
What happens after surgery is just as important as the procedure itself. To ensure the highest successful recovery, patients should follow these guidelines:
- Early Mobilization: Moving as soon as the doctor allows helps prevent blood clots.
- Neuro-Rehabilitation: Physical and occupational therapy can help the brain “re-learn” tasks if any pathways were disturbed.
- Healthy Nutrition: The brain requires high protein and healthy fats to repair its cellular structure.
- Mental Health Support: Recovery can be emotionally taxing; counseling or support groups play a huge role in long-term success.
When to Consult a Neurosurgeon
If you have been diagnosed with a growth or are experiencing unexplained neurological symptoms, time is of the essence. A successful outcome often depends on early intervention. You should seek an expert opinion if:
- Your symptoms are progressing rapidly.
- You want to explore minimally invasive options.
- You need a second opinion on a complex “inoperable” diagnosis. At العمود الفقري والدماغ الهند , we specialize in complex cases that require a high level of precision and personalized care.
Take the First Step Toward Recovery
Our neurosurgical experts use world-class technology to ensure the highest success rates and safety for our patients. Don’t navigate this journey alone.
حدد موعد استشارتكTrusted by 5,000+ patients for advanced brain and spine care.
استنتاج
حتي how successful is brain tumor surgery? The answer is more encouraging today than at any point in medical history. With survival rates for many tumors reaching over 90% and new technologies protecting vital brain functions, patients can look forward to meaningful lives post-surgery. Success is a partnership between a skilled neurosurgical team, advanced technology, and the patient’s commitment to recovery. By understanding the factors that influence outcomes, you can approach your treatment with confidence and clarity.
الأسئلة المتكررة
1. How successful is brain tumor surgery for benign tumors?
Success rates are excellent, often exceeding 90%. For many benign tumors, complete surgical removal is curative, allowing patients to return to a normal lifestyle with minimal risk of the tumor returning.
2. What factors most affect the surgical outcome?
Success depends on the tumor’s location, its size, and the patient’s overall health. Using advanced tools like neuronavigation (brain GPS) and intraoperative MRI significantly increases the chances of a successful removal.
3. Is surgery successful if the whole tumor isn’t removed?
Yes. Removing a large portion (debulking) is often considered a success. It reduces pressure on the brain, relieves symptoms like headaches or seizures, and helps subsequent treatments like radiation work more effectively.
4. What is the typical survival rate?
Survival varies by tumor grade. Benign tumors have a 5-year survival rate of over 90%. For malignant tumors, survival depends on the specific cell type, but modern treatments are consistently extending life expectancy and quality.
5. How long does recovery take?
Most patients see significant functional improvement within 6 to 12 weeks. While you may leave the hospital in a few days, the brain continues to heal and adapt for several months post-surgery.
6. Why is “awake surgery” used?
It is used for tumors near speech or movement centers. By keeping the patient awake to perform simple tasks, the surgeon can ensure vital functions remain intact, making the surgery much more successful in preserving quality of life.